Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder
Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder
Causes
The causes of Alzheimer’s Disease (AD) are multifaceted, involving a complex interplay of genetic, environmental, and lifestyle factors. While the exact etiology remains incompletely understood, several key contributors have been identified.
Genetic Factors: Genetic predisposition plays a significant role in the development of AD. Individuals with a family history of the disease are at an increased risk of developing it themselves. Specific genetic mutations, such as those in the amyloid precursor protein (APP), presenilin 1 (PSEN1), and presenilin 2 (PSEN2) genes, have been linked to familial forms of Alzheimer’s Disease, which typically manifest earlier in life.
Environmental Factors: Environmental influences also contribute to the risk of developing Alzheimer’s Disease. Cardiovascular health, for instance, plays a crucial role, as conditions like hypertension, high cholesterol, and diabetes are associated with an increased risk of AD. Additionally, factors such as education level, socioeconomic status, and exposure to toxins or pollutants may impact an individual’s susceptibility to the disease.
Lifestyle Factors: Certain lifestyle choices may influence the likelihood of developing Alzheimer’s Disease. Poor dietary habits, lack of physical activity, smoking, and excessive alcohol consumption have been identified as potential risk factors. Conversely, engaging in activities that promote brain health, such as regular exercise, a balanced diet rich in antioxidants and omega-3 fatty acids, and cognitive stimulation, may help reduce the risk of cognitive decline associated with AD.
Age: Advancing age is the most significant risk factor for Alzheimer’s Disease. While the disease can occur in younger individuals, the likelihood of developing it increases with age, particularly after the age of 65. This age-related increase in risk is thought to be due to a combination of genetic and environmental factors, as well as age-related changes in brain structure and function.
In summary, Alzheimer’s Disease arises from a complex interplay of genetic, environmental, and lifestyle factors, with advancing age being the most significant risk factor. Understanding these causes is crucial for developing targeted interventions aimed at reducing the burden of AD on individuals and society as a whole. (Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder)
Signs and Symptoms
Alzheimer’s Disease (AD) manifests through a spectrum of cognitive, behavioral, and functional changes, gradually eroding an individual’s ability to perform daily tasks and maintain independence. Recognizing the signs and symptoms of AD is crucial for early detection and intervention.

Memory Loss: One of the hallmark symptoms of Alzheimer’s Disease is memory impairment. Individuals may experience difficulty remembering recently learned information, important dates, or events. They may frequently repeat themselves or rely on memory aids to compensate for their forgetfulness.
Cognitive Decline: Alzheimer’s Disease affects various cognitive functions beyond memory. Individuals may struggle with language and communication, experiencing difficulty finding the right words or following conversations. They may also have impaired judgment, struggle with problem-solving tasks, and exhibit decreased attention and concentration.
Functional Impairment: As Alzheimer’s Disease progresses, individuals may find it increasingly challenging to perform routine tasks independently. Simple activities such as dressing, grooming, and managing finances may become overwhelming. In later stages, individuals may require assistance with basic activities of daily living, such as eating, bathing, and toileting.
Behavioral Changes: Alzheimer’s Disease can also lead to changes in behavior and personality. Individuals may become more withdrawn, apathetic, or agitated. They may exhibit mood swings, irritability, or aggression. Additionally, they may experience hallucinations, delusions, or paranoia as the disease progresses.
Loss of Spatial Awareness: In advanced stages of Alzheimer’s Disease, individuals may lose their sense of spatial awareness and become disoriented in familiar environments. They may have difficulty navigating their surroundings or recognizing familiar landmarks.
Social Withdrawal: Alzheimer’s Disease can also impact an individual’s social interactions and relationships. They may withdraw from social activities, lose interest in hobbies or previously enjoyed activities, and have difficulty maintaining meaningful connections with others.
Alzheimer’s Disease is characterized by a range of cognitive, behavioral, and functional changes that gradually worsen over time. Recognizing these signs and symptoms is crucial for early detection and diagnosis, allowing for timely intervention and support for individuals affected by this debilitating neurological disorder. (Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder)
Etiology
The etiology of Alzheimer’s Disease (AD) is complex and multifactorial, involving a combination of genetic, environmental, and lifestyle factors that contribute to the development and progression of the disease.
Genetic Factors: Genetic predisposition plays a significant role in the etiology of AD. Individuals with a family history of the disease are at an increased risk of developing it themselves, suggesting a hereditary component. Specific genetic mutations have been identified as contributing to the development of familial forms of Alzheimer’s Disease, which typically manifest earlier in life. Mutations in genes such as amyloid precursor protein (APP), presenilin 1 (PSEN1), and presenilin 2 (PSEN2) are associated with an increased risk of developing AD.
Environmental Factors: Environmental influences also contribute to the etiology of Alzheimer’s Disease. Cardiovascular health is closely linked to brain health, and conditions such as hypertension, high cholesterol, and diabetes increase the risk of developing AD. Additionally, factors such as education level, socioeconomic status, and exposure to toxins or pollutants may impact an individual’s susceptibility to the disease.
Lifestyle Factors: Certain lifestyle choices may influence the risk of developing Alzheimer’s Disease. Poor dietary habits, lack of physical activity, smoking, and excessive alcohol consumption have been identified as potential risk factors. Conversely, engaging in activities that promote brain health, such as regular exercise, a balanced diet rich in antioxidants and omega-3 fatty acids, and cognitive stimulation, may help reduce the risk of cognitive decline associated with AD.
Age: Advancing age is the most significant risk factor for Alzheimer’s Disease. While the disease can occur in younger individuals, the likelihood of developing it increases with age, particularly after the age of 65. This age-related increase in risk is thought to be due to a combination of genetic and environmental factors, as well as age-related changes in brain structure and function.
In summary, the etiology of Alzheimer’s Disease is multifaceted, involving a complex interplay of genetic, environmental, and lifestyle factors. Understanding these factors is crucial for identifying individuals at risk and developing targeted interventions to prevent or delay the onset of AD. (Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder)
Pathophysiology
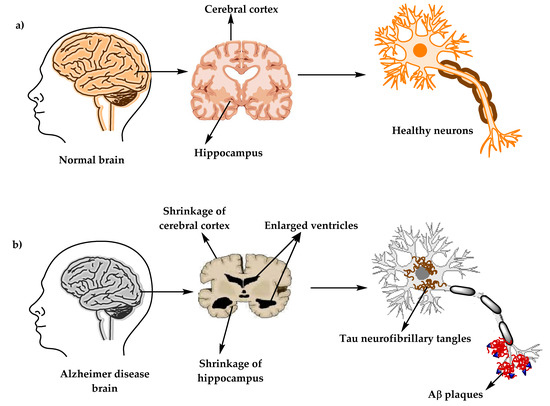
The pathophysiology of Alzheimer’s Disease (AD) involves complex changes in the structure and function of the brain, leading to progressive cognitive decline and neurological impairment. While the precise mechanisms underlying AD remain incompletely understood, several key pathological features have been identified.
Amyloid Plaques: One of the hallmark pathological features of Alzheimer’s Disease is the accumulation of beta-amyloid plaques in the brain. These plaques are formed by the abnormal aggregation of beta-amyloid protein fragments, which are derived from the cleavage of amyloid precursor protein (APP). The accumulation of beta-amyloid plaques disrupts neuronal function, leading to synaptic dysfunction and neuronal death.
Tau Tangles: Another characteristic feature of Alzheimer’s Disease is the formation of neurofibrillary tangles composed of hyperphosphorylated tau protein within neurons. Tau protein normally plays a crucial role in stabilizing microtubules within neurons. However, in AD, abnormal phosphorylation of tau leads to its aggregation into insoluble tangles, disrupting neuronal structure and function.
Neuronal Dysfunction: The accumulation of beta-amyloid plaques and tau tangles disrupts neuronal communication and impairs synaptic function, leading to cognitive dysfunction and memory impairment. Neuronal loss and synaptic degeneration further contribute to the progressive decline in cognitive function observed in AD.
Inflammatory Response: Inflammation also plays a significant role in the pathophysiology of Alzheimer’s Disease. Microglia, the immune cells of the central nervous system, become activated in response to the accumulation of beta-amyloid plaques and tau tangles, leading to chronic neuroinflammation. This inflammatory response contributes to neuronal damage and exacerbates neurodegeneration in AD.
Neurotransmitter Imbalance: Alterations in neurotransmitter levels, particularly acetylcholine and glutamate, are observed in Alzheimer’s Disease. Decreased levels of acetylcholine, a neurotransmitter involved in learning and memory, contribute to cognitive impairment. Excessive glutamate, an excitatory neurotransmitter, leads to neuronal excitotoxicity and further exacerbates neuronal damage in AD.
The pathophysiology of Alzheimer’s Disease involves complex interactions between amyloid plaques, tau tangles, neuronal dysfunction, neuroinflammation, and neurotransmitter imbalance. Understanding these pathological mechanisms is crucial for the development of targeted interventions aimed at slowing disease progression and improving outcomes for individuals affected by AD. (Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder)
DSM-5 Diagnosis
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), provides criteria for the diagnosis of Alzheimer’s Disease (AD). These criteria are based on clinical assessment and include the following key components:
Cognitive Decline: The DSM-5 criteria for AD require evidence of cognitive decline from a previous level of functioning. This decline must involve impairment in multiple cognitive domains, including memory, language, executive function, attention, and visuospatial abilities. The cognitive deficits must be severe enough to interfere with daily functioning and independence.
Gradual Onset and Progression: Alzheimer’s Disease is characterized by a gradual onset and progressive course of cognitive decline. The DSM-5 criteria specify that the cognitive deficits observed in AD should not be better explained by another neurocognitive disorder or a systemic condition that could cause cognitive impairment.
Significant Impairment in Daily Functioning: In addition to cognitive decline, the DSM-5 criteria require evidence of significant impairment in daily functioning due to the cognitive deficits associated with AD. This impairment may manifest as difficulties in performing routine activities of daily living, such as managing finances, preparing meals, or maintaining personal hygiene.
Exclusion of Other Causes: To establish a diagnosis of Alzheimer’s Disease, clinicians must rule out other potential causes of cognitive impairment, such as medical conditions, substance use, or medication side effects. The cognitive deficits observed in AD should not be attributable to another neurological or psychiatric disorder.
Diagnostic Criteria for Different Stages: The DSM-5 provides diagnostic criteria for both mild and major neurocognitive disorders due to Alzheimer’s Disease, reflecting the continuum of cognitive impairment associated with the disease. These criteria specify the severity of cognitive decline and its impact on daily functioning required for each stage of the disorder.
The DSM-5 diagnosis of Alzheimer’s Disease is based on clinical assessment and requires evidence of cognitive decline, gradual onset and progression, significant impairment in daily functioning, exclusion of other causes of cognitive impairment, and consideration of different stages of the disorder based on severity. These criteria facilitate the accurate diagnosis and classification of Alzheimer’s Disease, guiding appropriate treatment and management strategies for affected individuals. (Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder)
Treatment Regimens
While there is currently no cure for Alzheimer’s Disease (AD), various treatment regimens aim to manage symptoms, slow disease progression, and improve the quality of life for individuals affected by the disease.
Pharmacological Interventions: Pharmacological interventions are commonly used to alleviate symptoms and delay cognitive decline in Alzheimer’s Disease. Cholinesterase inhibitors, such as donepezil, rivastigmine, and galantamine, are often prescribed to improve cognitive function and alleviate symptoms of memory loss and confusion. Memantine, an N-methyl-D-aspartate (NMDA) receptor antagonist, is another medication used to regulate glutamate levels in the brain and improve cognitive function in individuals with moderate to severe AD.
Non-Pharmacological Interventions: Non-pharmacological interventions play a crucial role in managing Alzheimer’s Disease and improving the overall well-being of affected individuals. Cognitive stimulation therapy, reminiscence therapy, and reality orientation therapy are examples of non-pharmacological interventions aimed at improving cognitive function, enhancing communication, and promoting social engagement. Additionally, caregiver support programs provide education, resources, and emotional support to caregivers, helping them better cope with the challenges of caring for someone with AD.
Lifestyle Modifications: Lifestyle modifications, including regular physical exercise, a balanced diet, social engagement, and cognitive stimulation, are essential components of treatment regimens for Alzheimer’s Disease. Physical exercise has been shown to improve cognitive function, reduce the risk of cognitive decline, and enhance overall brain health. A balanced diet rich in antioxidants, omega-3 fatty acids, and vitamins may also help support brain function and reduce inflammation associated with AD.
Patient Education
Patient education plays a crucial role in empowering individuals with Alzheimer’s Disease and their caregivers to understand the nature of the disease, manage symptoms effectively, and make informed decisions about treatment and care.
Understanding Alzheimer’s Disease: Education about Alzheimer’s Disease helps individuals and their families understand the underlying mechanisms of the disease, its progression, and potential treatment options. By understanding the nature of the disease, individuals can better cope with the challenges of living with AD and make informed decisions about their care.
Managing Symptoms: Education about symptom management is essential for individuals with Alzheimer’s Disease and their caregivers. Learning strategies to manage symptoms such as memory loss, confusion, and changes in behavior can help individuals maintain their independence and quality of life for as long as possible.
Planning for the Future: Education about planning for the future is crucial for individuals with Alzheimer’s Disease and their families. This includes discussing advance care planning, legal and financial planning, and long-term care options. By planning, individuals can ensure their wishes are honored and their needs are met as the disease progresses.
Accessing Resources and Support: Education about available resources and support services is essential for individuals with Alzheimer’s Disease and their caregivers. This includes information about local support groups, respite care services, and community resources that can provide assistance and emotional support throughout the caregiving journey.
Treatment regimens for Alzheimer’s Disease encompass a combination of pharmacological and non-pharmacological interventions aimed at managing symptoms, slowing disease progression, and improving quality of life. Patient education is essential for empowering individuals and their caregivers to understand the disease, manage symptoms effectively, plan for the future, and access resources and support services to navigate the challenges of Alzheimer’s Disease with confidence and resilience. (Nursing Paper Example on Alzheimer’s Disease: Unveiling the Mysteries of a Neurological Disorder)




