Literature Review 5
(Literature Review 5)
Introduction
Falls are common in older adults, leading to serious injuries, including fractures and head injuries, and death in worst-case scenarios. Falls are also associated with disability and significant morbidity and mortality among older adults. Old age leads to overall poor physical and mental or cognitive status, which makes older adults prone to falls that cause physical injury and, in some instances, fear and psychological trauma. Statistically, a third of older adults experience at least one fall annually, while 10% fall multiple times yearly (Lloyd, 2021). Medical conditions increase the risk of falls, jeopardizing an older adult’s independence, and associated socioeconomic and personal consequences. Falls can occur at home or in any healthcare setting, including nursing homes. Hospitals are responsible for adopting interventions to minimize or prevent falls in older adults. Many interventions are adopted to prevent falls, including improving the environment and the terrain to make walking easy, providing non-slippery footwear, patient education, adequate lighting, installing handrails in hallways and bathrooms, and raising the bed to a comfortable height. This paper focuses on the role of hourly rounding in reducing the risk of falls among older adults. The paper explores literature offering evidence on the effectiveness of hourly rounding in preventing falls. (Literature Review 5)
Background
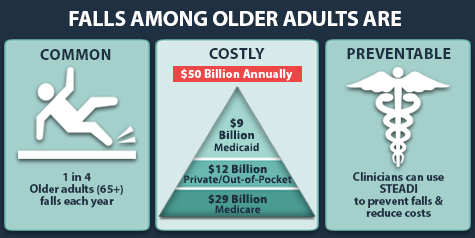
Falls among older adults are one of the most prevalent and dangerous issues causing disabilities, physical injury, and cognitive impairment. Falls are directly correlated with mortality, morbidity, and decreased functionality. Falls are widespread among the elderly, kids, and athletes. Studies have indicated that a higher tendency to fall and, thus, a higher risk of injury is connected with medical comorbidities in the elderly (Appeadu & Bordoni, 2022). Falls are also linked to socioeconomic and personal effects, including direct and indirect healthcare costs such as paying for fall-related injury treatment and financial loss from the patient’s or the caregiver’s work absence to attend to the injury or impaired functionality. According to Appeadu & Bordoni (2022), the US incurs over $31 billion, which could rise to 74 billion by 2030, associated with falls among older adults 65 years and over. Conclusively, falls impact the patient and the healthcare system in multiple ways, including increasing healthcare costs, contributing to medical conditions, financial loss, and impaired functionality. Therefore, it is critical to prevent falls and reduce the risk of falls for hospitalized patients to promote their quality of care.
Falls lead to different injuries, including minor and major fractures and head injuries. Approximately 30%-50% are minor, 10% major injuries, and 1% hip fractures, with the last one increasing post-fall morbidity and mortality risk. Approximately 20% lead to serious injuries, including fractures in other body parts or head injuries. Studies have shown that, annually, fall-related injuries lead to over 800,000 hospitalizations, with 300,000 requiring hip fracture treatment (Vaishya & Vaish, 2020). Falls are estimated to be the leading cause of traumatic brain injury and associated deaths among older people aged 65 years and above. Repeated falls increase the risk of severe injury, hospitalization, and death because of frail body structures (Vaishya & Vaish, 2020). About half of the falls lead to an injury, with major ones including head injuries and fractures. Frailty rather than age determines the severity of an injury and associated consequences. In conclusion, falls cause different types of injuries that can lead to morbidity, disability, loss of function, and mortality among older adults. Therefore, preventing falls and their associated injuries is critical to promote patient safety and experience during their hospital stay. (Literature Review 5)
PICOT Question
Among older patients, does patient education and hourly rounding reduce the risk of falls compared with normal nursing care?
Factors Most Frequently Associated with Falls in Elderly Patients
Inpatient falls, and fall-related injuries can be caused by various factors, including physical or cognitive impairments, environmental hazards, inadequate staff supervision, and age-related, such as hearing and vision impairment, vibration sensation and proprioceptive reduction, altered gait, and declining positional control. Age-related factors and changes do not cause falls directly but significantly contribute to most falls. Research shows that falls in older adults are also associated with physical diseases, medication side effects, cognitive deterioration, and environmental hazards (Vaishya & Vaish, 2020). According to Vaishya and Vaish (2020), environmental factors increase the risk of falling and can occur independently or interact with other factors, especially when postural control and mobility are needed, like walking on slippery and uneven surfaces. Maintaining balance becomes a problem as people age because of an impaired nervous system, which makes recovering balance challenging (Cuevas-Trisan, 2019). Furthermore, older age causes muscle weaknesses that make balancing and positioning difficult, leading to increased fall risk. Also, inadequate staffing or insufficient staff supervision can mean potential fall risks are not identified and addressed quickly enough (Vaishya & Vaish, 2020). In conclusion, inpatient falls, and fall-related injuries can be caused by a variety of factors, including physical or cognitive impairments, environmental hazards, and inadequate staff supervision. It is important to identify these potential causes to reduce the risk of falls and fall-related injuries. (Literature Review 5)
Impact of Fall Prevention Programs on Number of Falls Experienced by Elderly Patients
Falls prevention programs are implemented to reduce the risk of falls and fall-related injuries among hospitalized patients, especially older patients. There are many fall prevention programs, including reorganizing the Falls Committee, flagging high-risk patients, improving fall reports, increasing falls scrutiny, adopting hourly nursing rounds, reorganizing leadership systems, standardizing fall prevention equipment, adapting to new hospital buildings, investigating root causes, educating patients, and helping nurses think critically regarding risk. Additionally, falls prevention interventions can include alarms, fall risk identification, sitters, intentional rounding, patient education, physical restraints, environmental modifications, and non-slip socks. Studies indicate that fall prevention programs have varying effectiveness, but using several interventions at once increases the efficacy of fall prevention efforts. Based on research, hourly rounding generates consistent fall prevention results and reduces risk factors associated with falls among older adults. According to Daniels (2016), purposeful and timely hourly rounding is one of the effective nursing interventions to meet patient needs consistently, ensuring patient safety, lowering preventable events, and proactively addressing patient problems. According to the Institute for Healthcare Improvement (IHI), hourly rounding is the best approach to prevent and minimize call lights and fall injuries, increasing care quality and patient satisfaction. The study recommends increasing nurse knowledge on purposeful hourly rounding and facilitating infrastructure to ensure consistency with this intervention. Mant et al. (2016) also found that implementing hourly rounding effectively prevents fall-related incidents among older patients in acute care settings. Goldsack (2015) found that the effectiveness of hourly rounding in preventing patient falls depends on multiple factors, such as staff training, interdisciplinary teams, and leadership. Goldsack (2015) found that the unit that engaged staff and leadership in the project achieved a 3.9 falls/1000 patient days, with the pilot period fall rate being considerably lower, at 1.3 falls/1,000 patient days. In the second unit, the fall rate was 2.6 falls per 1000 patient days and 2.5 falls per 1000 patient days during the pilot period. These findings indicate that adopting an interdisciplinary team that includes leadership and unit champions can enhance the effectiveness of a patient-centered proactive hourly rounding program, leading to significant fall rate reduction. Therefore, leadership and front-line staff should be actively involved in developing and implementing hourly rounding programs. Walsh et al. (2018) explored the effectiveness of reorganizing the Falls Committee, flagging high-risk patients, improving fall reports, increasing falls scrutiny, adopting hourly nursing rounds, reorganizing leadership systems, standardizing fall prevention equipment, adapting to the new hospital building, investigating root causes, educating patients, and helping nurses think critically regarding risk in reducing patient falls. These interventions reduced the fall rate from 3.07 to 2.22 per 1000 patient days and injury reduction from 0.77 to 0.65 per 1000 patient days. When nurses began addressing fall risk during hourly rounds, the fall rate significantly declined, implying hourly rounds’ effectiveness in reducing the fall risk among inpatients. Heng et al. (2020) explored the effectiveness of patient education in preventing falls among older adults. Findings indicate that direct face-to-face patient education, educational materials like handouts, pamphlets, brochures, hospital policies, procedures, and systems can help reduce falls and associated injuries. Fall prevention programs incorporating patient education reduce the risk of falling because patients are empowered and more aware of themselves and their surroundings. Heng et al. (2021) also explored patient education’s impact on fall rate and found that consistent, patient-centered education and small interactive groups helped prevent falls among hospitalized patients. LeLaurin & Shorr (2019) investigated the effectiveness of alarms, fall risk identification, sitters, intentional rounding, patient education, physical restraints, environmental modifications, and non-slip socks. LeLaurin & Shorr (2019) found that intentional rounding enhances patient satisfaction and minimizes patient harm. It is a proactive method that helps meet patient needs, involving bedside checks and schedule intervals, typically one hour during the day and after two hours during the night. However, inadequate education, workload, lack of staff adherence, competing priorities, and poor documentation can be barriers to intentional hourly rounding. Consistently, Manges et al. (2020) found that hourly rounding improved care quality, patient satisfaction, and patient empowerment and helped decrease patient fall rates. In conclusion, multiple fall prevention programs are implemented in hospitals, but research shows most fall prevention programs have moderate effects on fall prevention. However, hourly rounding and patient education significantly reduce the risk of falls and associated injuries. Therefore, hospitals should consider adopting purposeful and intentional hourly rounding and patient education to prevent falls among older patients. Falls prevention patient education can be incorporated during hourly rounding to increase the effectiveness of fall prevention efforts. (Literature Review 5)
Impact of Medication Management on Fall Prevention in Elderly Patients
Hospitalized patients, particularly older adults, are under several medications, which increases the risk of medication-induced falls. Medication side effects that increase the risk of falling are often ignored, and fall-risk-increasing drugs should be considered a significant risk factor during fall risk assessment in healthcare settings. Research shows that about 47% of active substances used by inpatients increase the risk of falling because most affect the nervous and cardiovascular systems (Michalcova et al., 2020). The findings recommend adopting medication management programs such as preliminary categorizing fall-risk-increasing drugs (FRIDs) based on adverse drug effects to reduce fall risk. Ming et al. (2021) report medication review as an effective approach to managing adverse drug reactions and enhancing drug safety among older patients. According to Ming et al. (2021), medication review effectively prevents falls and fall-related injuries among older adults. Medication review also helped reduce the severity of injuries and fall-related fractures. In conclusion, there are different medication management programs, including risk categorization of drugs according to their adverse effects and medication review of drugs that can help prevent medication-induced falls. Therefore, hospitals should increase awareness of medication-induced falls and adopt medication management programs to prevent falls and fall-related injuries. (Literature Review 5)
Conclusion
Patient falls are a significant problem in US hospitals, especially among older adults at increased risk of falling due to age-related factors, environmental factors, medical conditions, and frail bodies. Falls lead to injuries and contribute considerably to subsequent morbidity and mortality among hospitalized patients. Many interventions currently used to prevent falls indicate moderate benefits and unknown sustainability. Reviewed articles provide consistent results showing patient education and hourly rounding as effective in reducing the risk of patient falls, promoting patient safety, and improving patient experience, outcome, and satisfaction. (Literature Review 5)
References
Appeadu, M. K., & Bordoni, B. (2022). Falls and fall prevention in the elderly. In StatPearls [Internet]. StatPearls Publishing.
Cuevas-Trisan, R. (2019). Balance problems and fall risks in the elderly. Clinics in geriatric medicine, 35(2), 173-183.
Daniels J. F. (2016). Purposeful and timely nursing rounds: a best practice implementation project. JBI database of systematic reviews and implementation reports, 14(1), 248–267. https://doi.org/10.11124/jbisrir-2016-2537
Goldsack, J., Bergey, M., Mascioli, S., & Cunningham, J. (2015). Hourly rounding and patient falls: what factors boost success?. Nursing, 45(2), 25–30. https://doi.org/10.1097/01.NURSE.0000459798.79840.95
Heng, H., Jazayeri, D., Shaw, L., Kiegaldie, D., Hill, A. M., & Morris, M. E. (2020). Hospital falls prevention with patient education: a scoping review. BMC geriatrics, 20(1), 140. https://doi.org/10.1186/s12877-020-01515-w
Heng, H., Slade, S. C., Jazayeri, D., Jones, C., Hill, A. M., Kiegaldie, D., Shorr, R. I., & Morris, M. E. (2021). Patient Perspectives on Hospital Falls Prevention Education. Frontiers in public health, 9, 592440. https://doi.org/10.3389/fpubh.2021.592440
LeLaurin, J. H., & Shorr, R. I. (2019). Preventing Falls in Hospitalized Patients: State of the Science. Clinics in geriatric medicine, 35(2), 273–283. https://doi.org/10.1016/j.cger.2019.01.007
Lloyd, S. L. (2021). Hourly rounding to reduce patient falls – A quality improvement project. University of Texas.
Manges, M. E., Zuver, M. C., Mack, K., & Abraham, S. P. (2020). hourly rounding and medical-surgical patient falls: A review of the literature. International Journal of Science and Research Methodology.
Mant, T., Dunning, T., & Hutchinson, A. (2016). The clinical effectiveness of hourly rounding on fall-related incidents involving adult patients in an acute care setting: a systematic review. JBI Evidence Synthesis, 10(56), 1-12.
Michalcova, J., Vasut, K., Airaksinen, M., & Bielakova, K. (2020). Inclusion of medication-related fall risk in fall risk assessment tool in geriatric care units. BMC geriatrics, 20(1), 1-11.
Ming, Y., Zecevic, A. A., Hunter, S. W., Miao, W., & Tirona, R. G. (2021). Medication Review in Preventing Older Adults’ Fall-Related Injury: a Systematic Review & Meta-Analysis. Canadian geriatrics journal : CGJ, 24(3), 237–250. https://doi.org/10.5770/cgj.24.478
Vaishya, R., & Vaish, A. (2020). Falls in Older Adults are Serious. Indian journal of orthopaedics, 54(1), 69–74. https://doi.org/10.1007/s43465-019-00037-x
Walsh, C. M., Liang, L. J., Grogan, T., Coles, C., McNair, N., & Nuckols, T. K. (2018). Temporal Trends in Fall Rates with the Implementation of a Multifaceted Fall Prevention Program: Persistence Pays Off. Joint Commission journal on quality and patient safety, 44(2), 75–83. https://doi.org/10.1016/j.jcjq.2017.08.009
(Literature Review 5)
Do you need a similar assignment done for you from scratch? Order now!
Use Discount Code "Newclient" for a 15% Discount!