Nursing Paper Example on Beriberi Disease: Understanding Causes, Symptoms, and Treatment
Nursing Paper Example on Beriberi Disease: Understanding Causes, Symptoms, and Treatment
Causes
Beriberi disease arises primarily due to thiamine (vitamin B1) deficiency, essential for cellular metabolism and neurological function. This deficiency often stems from inadequate dietary intake, particularly in regions reliant on polished rice as a staple food, where thiamine-rich outer layers are removed during processing. Furthermore, certain dietary habits, such as excessive consumption of refined carbohydrates or alcohol, can exacerbate thiamine deficiency. Chronic alcoholism, in particular, predisposes individuals to Beriberi by interfering with thiamine absorption and utilization, as well as promoting poor dietary choices.
Moreover, malabsorption syndromes, such as celiac disease or inflammatory bowel diseases, can impair thiamine absorption in the gastrointestinal tract, leading to deficiency states. Additionally, increased metabolic demands during pregnancy and lactation can deplete thiamine stores, especially in populations with already marginal nutritional status. Certain medical conditions, including hyperemesis gravidarum and prolonged parenteral nutrition, can further contribute to thiamine depletion.
Furthermore, cultural and socioeconomic factors play a significant role in Beriberi prevalence. Communities relying heavily on polished rice as a dietary staple, without access to diverse and nutrient-rich foods, are at heightened risk of developing thiamine deficiency. Economic disparities and food insecurity exacerbate this risk, as marginalized populations may lack access to adequate nutrition and healthcare services. (Nursing Paper Example on Beriberi Disease: Understanding Causes Symptoms and Treatment)
In regions where food fortification and supplementation programs are limited or nonexistent, Beriberi prevalence remains a persistent public health challenge. Addressing the root causes of thiamine deficiency requires multifaceted approaches, including nutritional education, supplementation initiatives, and broader socioeconomic interventions to improve access to diverse and balanced diets. By understanding the intricate web of factors contributing to Beriberi, healthcare practitioners and policymakers can implement targeted strategies to mitigate its prevalence and alleviate the burden on affected populations.
Signs and Symptoms (Nursing Paper Example on Beriberi Disease: Understanding Causes Symptoms and Treatment)
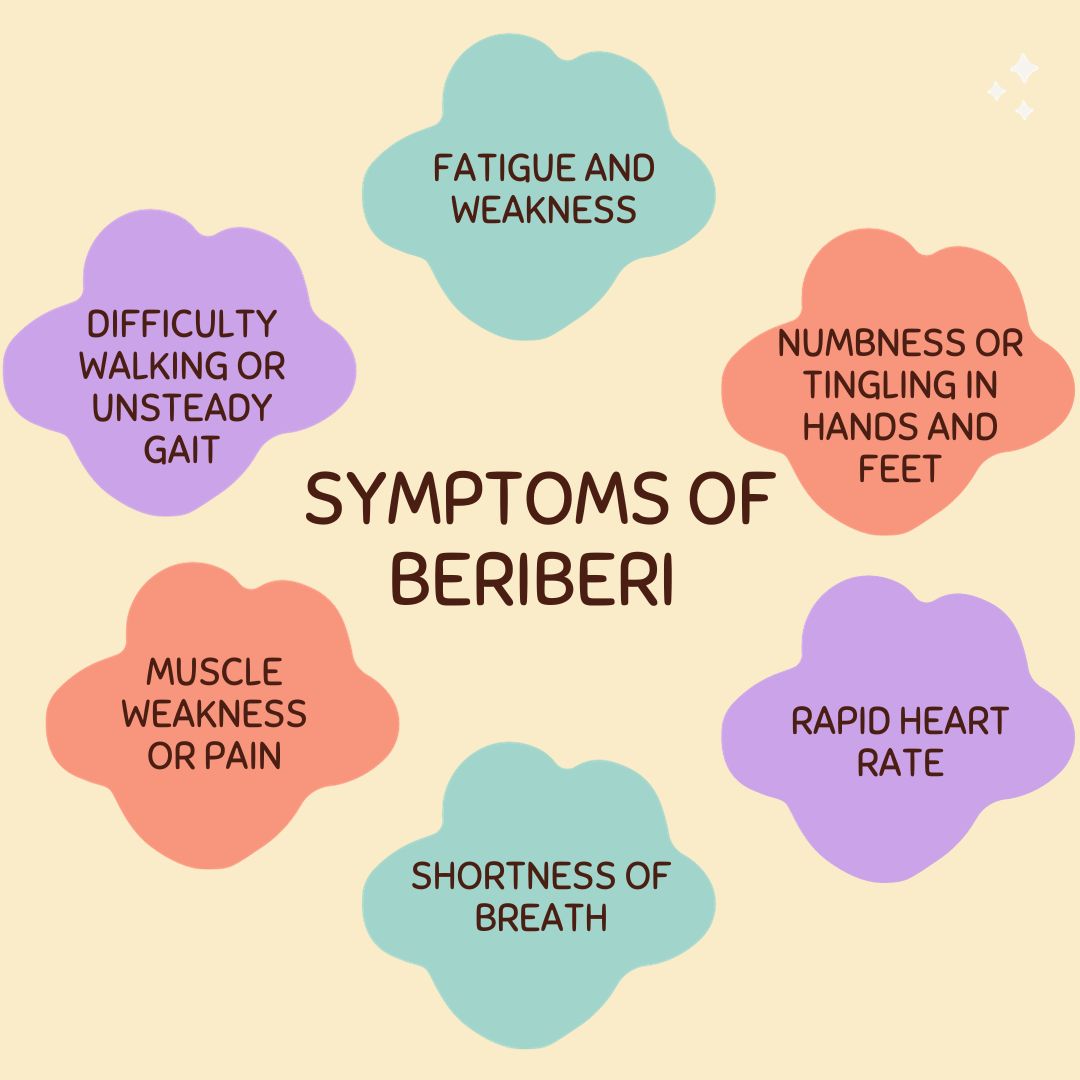
Beriberi: Causes, Risk Factors, Symptoms, Treatment
The clinical presentation of Beriberi disease varies depending on the affected systems, manifesting as either dry or wet beriberi. Dry beriberi predominantly affects the nervous system, resulting in symptoms such as muscle weakness, tingling sensations, and peripheral neuropathy. Patients may experience progressive weakness and fatigue, often exacerbated by physical exertion. Sensory disturbances, including numbness and tingling in the extremities, commonly occur due to peripheral nerve damage. Moreover, muscle wasting and decreased reflexes are characteristic features of dry beriberi, reflecting underlying neurological dysfunction.
Conversely, wet beriberi primarily targets the cardiovascular system, leading to symptoms like edema, tachycardia, and heart failure. Peripheral edema, particularly in the lower extremities, is a hallmark feature of wet beriberi, resulting from fluid accumulation due to impaired cardiac function. Patients may also exhibit symptoms of heart failure, including dyspnea, orthopnea, and paroxysmal nocturnal dyspnea, secondary to myocardial dysfunction and pulmonary congestion. Tachycardia and palpitations are common cardiovascular manifestations, reflecting the heart’s compensatory response to decreased cardiac output.
Furthermore, individuals with acute fulminant beriberi may present with profound cardiovascular collapse and cardiogenic shock, necessitating urgent medical intervention. The clinical spectrum of Beriberi disease encompasses a wide range of symptoms, varying in severity and presentation based on the underlying nutritional deficiency and physiological disturbances. Timely recognition and intervention are crucial to prevent disease progression and mitigate associated complications. Healthcare providers should maintain a high index of suspicion for Beriberi, especially in populations at risk of thiamine deficiency, and initiate appropriate diagnostic and therapeutic measures promptly. By addressing the diverse array of symptoms associated with Beriberi disease, healthcare practitioners can improve patient outcomes and enhance overall quality of life for affected individuals.
Etiology
The etiology of Beriberi disease is intricately linked to thiamine (vitamin B1) deficiency, which disrupts crucial metabolic pathways essential for cellular energy production and nerve conduction. Various factors contribute to thiamine deficiency, including poor dietary intake, malabsorption disorders, excessive alcohol consumption, and increased metabolic demands during pregnancy or lactation.
Inadequate dietary intake represents the primary etiological factor in regions where polished rice serves as a staple food. The removal of thiamine-rich outer layers during rice processing significantly reduces thiamine content, leading to widespread deficiency in populations reliant on this staple. Additionally, dietary habits emphasizing refined carbohydrates over nutrient-dense foods contribute to thiamine depletion, further exacerbating deficiency states.
Malabsorption syndromes, such as celiac disease, Crohn’s disease, and tropical sprue, impair thiamine absorption in the gastrointestinal tract, leading to deficiency states despite adequate dietary intake. Furthermore, chronic alcoholism poses a significant risk factor for Beriberi by interfering with thiamine absorption, metabolism, and utilization. Alcohol-induced gastritis and pancreatic dysfunction further exacerbate thiamine deficiency, contributing to the development of Beriberi in susceptible individuals.
Pregnancy and lactation impose increased metabolic demands, depleting thiamine stores and predisposing women to deficiency states, especially in populations with marginal nutritional status. Hyperemesis gravidarum, a severe form of nausea and vomiting during pregnancy, can exacerbate thiamine deficiency due to fluid and electrolyte imbalances. Prolonged parenteral nutrition, devoid of adequate thiamine supplementation, also poses a risk for thiamine depletion, particularly in hospitalized patients. (Nursing Paper Example on Beriberi Disease: Understanding Causes Symptoms and Treatment)
Moreover, socioeconomic factors, including poverty, food insecurity, and limited access to healthcare, exacerbate thiamine deficiency in vulnerable populations. Addressing the multifactorial etiology of Beriberi disease requires comprehensive interventions targeting dietary education, supplementation initiatives, and broader socioeconomic reforms to improve access to nutrient-rich foods and healthcare services.
Pathophysiology(Nursing Paper Example on Beriberi Disease: Understanding Causes Symptoms and Treatment)
The pathophysiology of Beriberi disease revolves around the multifaceted role of thiamine (vitamin B1) in cellular metabolism and neurological function. Thiamine serves as a crucial cofactor for several enzymes involved in carbohydrate metabolism, including the pyruvate dehydrogenase complex and alpha-ketoglutarate dehydrogenase complex. These enzymes play pivotal roles in converting pyruvate and alpha-ketoglutarate into acetyl-CoA and succinyl-CoA, respectively, initiating the citric acid cycle and facilitating ATP production through oxidative phosphorylation.
Thiamine deficiency disrupts these metabolic pathways, leading to dysfunctional energy production and accumulation of toxic byproducts. The impaired activity of the pyruvate dehydrogenase complex results in the accumulation of pyruvate and lactate, leading to lactic acidosis and metabolic acidosis. Furthermore, decreased acetyl-CoA production impairs lipid metabolism, contributing to fatty infiltration of the liver and other organs observed in severe cases of Beriberi disease.
Moreover, thiamine deficiency adversely affects neurological function by disrupting neurotransmitter synthesis and nerve conduction. Thiamine plays a crucial role in synthesizing acetylcholine, gamma-aminobutyric acid (GABA), and other neurotransmitters essential for neuronal signaling. Thiamine deficiency leads to impaired neurotransmitter synthesis, resulting in neuronal dysfunction and the manifestation of neurological symptoms such as muscle weakness, sensory disturbances, and peripheral neuropathy. (Nursing Paper Example on Beriberi Disease: Understanding Causes, Symptoms, and Treatment)
Additionally, thiamine deficiency disrupts myelin synthesis and maintenance, further compromising nerve conduction and contributing to peripheral neuropathy. The multifaceted pathophysiology of Beriberi disease underscores the systemic impact of thiamine deficiency on cellular metabolism and neurological function. Targeted interventions aimed at restoring thiamine levels and addressing metabolic derangements are essential for mitigating the clinical manifestations and associated complications of Beriberi disease.




