Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED]
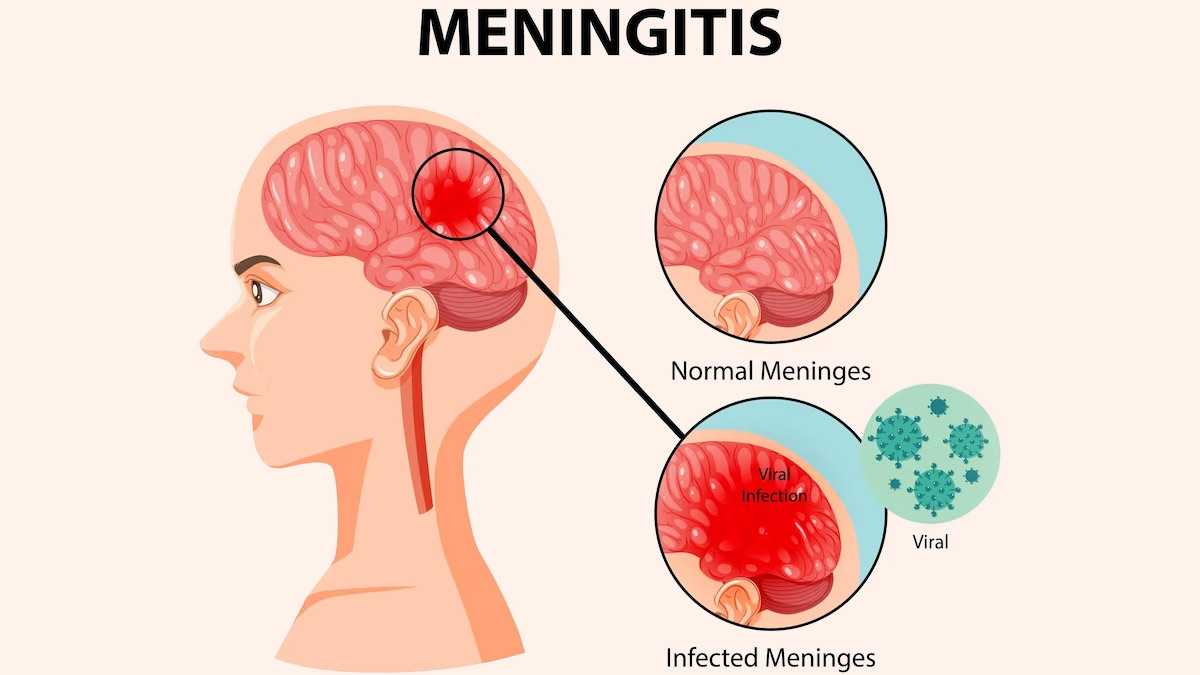
Encephalitis, an inflammation of the brain tissue, poses a significant medical challenge due to its potential for severe neurological complications. This paper endeavors to provide a comprehensive overview of encephalitis, focusing on its causes, symptoms, etiology, pathophysiology, DSM-5 diagnosis, treatment regimens, and patient education. Understanding the complexities of encephalitis is crucial for healthcare professionals to effectively manage this condition and optimize patient outcomes. From viral infections such as herpes simplex virus and West Nile virus to autoimmune reactions and bacterial etiologies, the causes of encephalitis are diverse and multifactorial. Recognizing the signs and symptoms, which can range from mild headache and confusion to severe neurological dysfunction, is paramount for early diagnosis and intervention. By delving into the pathophysiological mechanisms underlying encephalitis and exploring current treatment modalities, this paper aims to enhance healthcare providers’ understanding and management of this challenging neurological disorder. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
![Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED]](https://upload.wikimedia.org/wikipedia/commons/5/59/Viral_encephalitis.png)
Causes
Encephalitis can arise from various factors, predominantly viral infections. Among these, the herpes simplex virus (HSV) stands out as a common culprit, particularly HSV-1, which typically causes oral lesions but can also lead to encephalitis. Additionally, mosquito-borne viruses pose a significant risk, with West Nile virus (WNV) being a notable example. This virus, transmitted through mosquito bites, can infiltrate the central nervous system, inducing inflammation and neurological complications. Other viral agents implicated in encephalitis include the varicella-zoster virus (VZV), responsible for chickenpox and shingles, and the enteroviruses, which encompass a diverse group causing various illnesses, including meningitis and encephalitis.
Beyond viral etiologies, bacterial infections can also trigger encephalitis. Pathogens such as Streptococcus pneumoniae and Neisseria meningitidis can infiltrate the brain tissue, leading to inflammation and neurological symptoms. Parasitic infections, though less common, represent another potential cause of encephalitis. Parasites such as Toxoplasma gondii and Trypanosoma cruzi can invade the central nervous system, provoking an inflammatory response and neurological dysfunction.
Furthermore, non-infectious factors, particularly autoimmune reactions, can contribute to the development of encephalitis. Autoimmune encephalitis occurs when the body’s immune system mistakenly targets proteins in the brain, leading to inflammation and neurological impairment. Conditions such as anti-NMDA receptor encephalitis and Hashimoto’s encephalitis exemplify autoimmune-mediated forms of the disease.
Overall, the causes of encephalitis are diverse and multifaceted, encompassing viral, bacterial, parasitic, and autoimmune etiologies. Recognizing the various pathogens and mechanisms underlying encephalitis is crucial for accurate diagnosis and appropriate management strategies. Moreover, understanding the epidemiology and risk factors associated with each causative agent is essential for implementing preventive measures and mitigating the burden of this potentially devastating neurological disorder. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
Signs and Symptoms
The presentation of encephalitis can vary widely, ranging from mild flu-like symptoms to severe neurological impairment. One of the hallmark signs of encephalitis is fever, often accompanied by headache, which may be persistent and severe. Patients may also experience altered mental status, ranging from confusion and disorientation to profound lethargy or coma. Additionally, seizures are common in individuals with encephalitis, manifesting as abnormal electrical activity in the brain and often presenting as focal or generalized convulsions. Neurological deficits such as weakness, sensory disturbances, and coordination difficulties may also occur, reflecting the involvement of specific brain regions.
Behavioral changes are another notable feature of encephalitis, with patients exhibiting irritability, agitation, or personality alterations. Furthermore, speech and language impairments may arise, including difficulty articulating words or understanding language. In severe cases, encephalitis can lead to cranial nerve dysfunction, resulting in visual disturbances, hearing loss, or facial weakness.
Children with encephalitis may exhibit distinct symptoms, including irritability, poor feeding, and changes in sleep patterns. Additionally, infants may present with bulging fontanelles, a sign of increased intracranial pressure, and may demonstrate high-pitched crying or excessive fussiness.
In some instances, encephalitis can progress rapidly, leading to life-threatening complications such as respiratory failure or cardiovascular collapse. Prompt recognition of the signs and symptoms of encephalitis is critical for timely intervention and management. Healthcare providers should maintain a high index of suspicion, particularly in individuals with risk factors such as recent viral infections or immunocompromised states. Early diagnosis and initiation of treatment can significantly improve outcomes and reduce the risk of long-term neurological sequelae associated with encephalitis. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
Etiology
Encephalitis can arise from a myriad of etiological factors, reflecting the diverse nature of this neurological disorder. Viral infections represent the predominant cause of encephalitis, with numerous viruses capable of infiltrating the brain tissue and inducing inflammation. Herpes simplex virus (HSV) is a primary viral culprit, particularly HSV-1, which commonly causes oral lesions but can also lead to encephalitis, especially in immunocompromised individuals. Additionally, mosquito-borne viruses pose a significant risk, with West Nile virus (WNV) being a notable example. This virus, transmitted through mosquito bites, can breach the blood-brain barrier and initiate an inflammatory response within the central nervous system.
Bacterial infections also contribute to the etiology of encephalitis, albeit less frequently than viral pathogens. Bacteria such as Streptococcus pneumoniae and Neisseria meningitidis can invade the brain tissue, either directly or through hematogenous spread, leading to inflammation and neurological dysfunction.
Parasitic infections, though less common, represent another potential cause of encephalitis. Parasites such as Toxoplasma gondii and Trypanosoma cruzi can invade the central nervous system, eliciting an inflammatory response and neurological impairment.
Furthermore, non-infectious factors, particularly autoimmune reactions, play a significant role in the etiology of encephalitis. Autoimmune encephalitis occurs when the body’s immune system erroneously targets proteins in the brain, resulting in inflammation and neurological dysfunction. Conditions such as anti-NMDA receptor encephalitis and Hashimoto’s encephalitis exemplify autoimmune-mediated forms of the disease.
Overall, the etiology of encephalitis is multifactorial, encompassing viral, bacterial, parasitic, and autoimmune mechanisms. Understanding the diverse etiological factors contributing to encephalitis is crucial for accurate diagnosis and appropriate management strategies tailored to the underlying cause of the disease. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
Pathophysiology
The pathophysiology of encephalitis involves complex interactions between infectious agents, the immune system, and the central nervous system (CNS), culminating in inflammation and neuronal dysfunction. In viral encephalitis, viral particles gain access to the CNS either by breaching the blood-brain barrier or by traveling along neuronal pathways. Once within the brain tissue, viruses replicate and initiate an immune response, triggering the release of pro-inflammatory cytokines and chemokines. This inflammatory cascade recruits immune cells, including macrophages and lymphocytes, to the site of infection, where they attempt to control viral replication but may also contribute to tissue damage.
Bacterial encephalitis follows a similar pattern, with bacteria invading the CNS either directly or through hematogenous spread. Once in the brain tissue, bacteria release toxins and activate the host immune response, leading to inflammation and tissue injury. The inflammatory process disrupts normal neuronal function and can result in the manifestation of neurological symptoms.
In autoimmune encephalitis, the pathophysiology involves an aberrant immune response directed against self-antigens within the CNS. Autoantibodies produced by the immune system target specific proteins on neuronal cells, leading to neuronal dysfunction and inflammation. This autoimmune-mediated damage disrupts synaptic transmission and neuronal signaling, contributing to the development of neurological symptoms characteristic of encephalitis.
Overall, the pathophysiology of encephalitis is characterized by a complex interplay between infectious agents, immune responses, and neuronal dysfunction. Understanding the underlying mechanisms driving the inflammatory process is crucial for developing targeted therapeutic interventions aimed at mitigating tissue damage and improving patient outcomes. Further research into the pathophysiological pathways involved in encephalitis may uncover novel therapeutic targets and strategies for the management of this challenging neurological disorder. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
DSM-5 Diagnosis
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), provides criteria for diagnosing encephalitis-related psychiatric symptoms, facilitating accurate assessment and treatment planning. While encephalitis primarily presents with neurological manifestations, psychiatric symptoms can also occur, ranging from mild cognitive deficits to severe behavioral disturbances. According to DSM-5 criteria, encephalitis-related psychiatric symptoms may include alterations in mood, cognition, and behavior that are not better explained by another mental disorder or medical condition.
One of the key features indicative of encephalitis-related psychiatric symptoms is the presence of acute onset, with symptoms emerging shortly after the onset of neurological dysfunction. Patients may exhibit mood disturbances such as irritability, agitation, or emotional lability, which can fluctuate in intensity and duration. Cognitive deficits, including impaired attention, memory disturbances, and disorientation, may also be evident, reflecting the underlying disruption of normal brain function. Additionally, behavioral changes such as impulsivity, disinhibition, or psychosis may occur, further complicating the clinical presentation.
The DSM-5 emphasizes the importance of conducting a thorough clinical assessment to differentiate encephalitis-related psychiatric symptoms from primary psychiatric disorders or other medical conditions. This includes obtaining a comprehensive medical history, conducting neurological examinations, and performing relevant laboratory tests and imaging studies to rule out alternative etiologies.
Overall, the DSM-5 provides valuable guidance for clinicians in diagnosing and managing encephalitis-related psychiatric symptoms, facilitating early intervention and appropriate treatment. By recognizing the psychiatric manifestations of encephalitis and distinguishing them from other mental health conditions, healthcare providers can optimize patient care and improve outcomes for individuals affected by this challenging neurological disorder. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
Treatment Regimens and Patient Education
Effective management of encephalitis requires a multifaceted approach encompassing pharmacological interventions, supportive care, and patient education to optimize outcomes and minimize complications. Treatment regimens for encephalitis are tailored to the underlying etiology and severity of symptoms, with the primary goals of controlling inflammation, managing symptoms, and preventing long-term neurological sequelae.
Pharmacological interventions play a central role in the treatment of encephalitis, particularly in cases caused by viral or autoimmune etiologies. Antiviral medications, such as acyclovir or ganciclovir, are commonly prescribed for viral encephalitis to inhibit viral replication and reduce the severity of symptoms. Corticosteroids may also be utilized to suppress inflammation and modulate the immune response, particularly in cases of autoimmune encephalitis.
In addition to antiviral and immunomodulatory therapies, supportive care is essential in managing the symptoms and complications of encephalitis. This may include symptomatic relief for headache, fever, and seizures, as well as nutritional support and hydration to maintain adequate fluid and electrolyte balance. In severe cases, patients may require intensive care monitoring and respiratory support to prevent respiratory failure or other life-threatening complications.
Patient education plays a vital role in the management of encephalitis, empowering individuals and their caregivers to actively participate in their care and recovery. Education should encompass various aspects, including the importance of adherence to prescribed medications, recognition of warning signs of worsening symptoms, and strategies for preventing complications. Patients and caregivers should be educated about the potential side effects of medications and instructed on when to seek medical attention.
Furthermore, patients should be counseled on lifestyle modifications to support recovery and promote overall well-being. This may include recommendations for adequate rest, balanced nutrition, and regular physical activity within the limits of their condition. Additionally, patients should be advised to avoid activities that may increase the risk of injury, such as driving or operating heavy machinery, until cleared by their healthcare provider.
Overall, a comprehensive approach to treatment and patient education is essential in optimizing outcomes for individuals affected by encephalitis. By addressing the diverse needs of patients and caregivers and promoting active engagement in care, healthcare providers can enhance the quality of life and long-term prognosis for individuals recovering from this challenging neurological disorder. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
Conclusion
Encephalitis presents a multifaceted challenge requiring a comprehensive understanding of its causes, symptoms, and treatment modalities. By elucidating the diverse etiological factors contributing to encephalitis, including viral, bacterial, parasitic, and autoimmune mechanisms, healthcare providers can tailor treatment regimens to address the underlying pathology. Moreover, recognizing the varied clinical manifestations of encephalitis, from neurological deficits to psychiatric symptoms, facilitates timely diagnosis and intervention. Through pharmacological interventions, supportive care, and patient education, individuals affected by encephalitis can receive optimal management aimed at controlling inflammation, managing symptoms, and preventing long-term complications. The inclusion of detailed discussions on pathophysiology, DSM-5 diagnosis, treatment regimens, and patient education ensures a comprehensive overview of encephalitis, empowering healthcare providers to deliver informed and effective care. Overall, this paper underscores the importance of a multidisciplinary approach to encephalitis management, emphasizing the need for ongoing research, education, and collaboration to improve outcomes for individuals affected by this challenging neurological disorder. (Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED])
References
https://www.ncbi.nlm.nih.gov/books/NBK470162/


![Nursing Paper Example on Encephalitis: Causes, Symptoms, and Treatment [SOLVED]](https://upload.wikimedia.org/wikipedia/commons/5/59/Viral_encephalitis.png)
